Stress, Brain & Trauma-Sensitive Mindfulness

Stress and the brain
Stress is simply the body’s response to change, and not all stress is bad.
To understand what might be happening when you are stressed, triggered or caught up in difficult emotions (for example, anger, fear, anxiety), a basic understanding of the brain can be helpful.
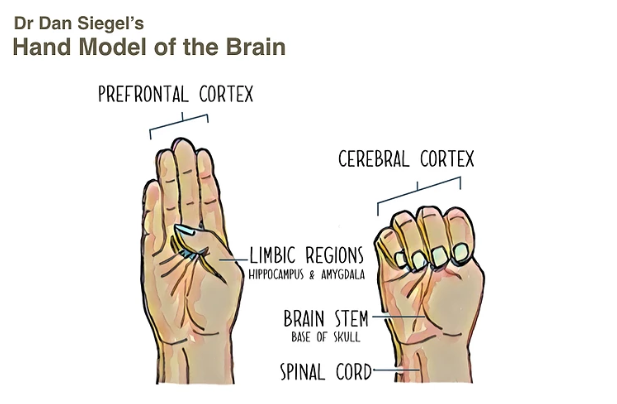
Here’s a 8 min video of Dr. Dan Siegel explaining the hand model of the brain:
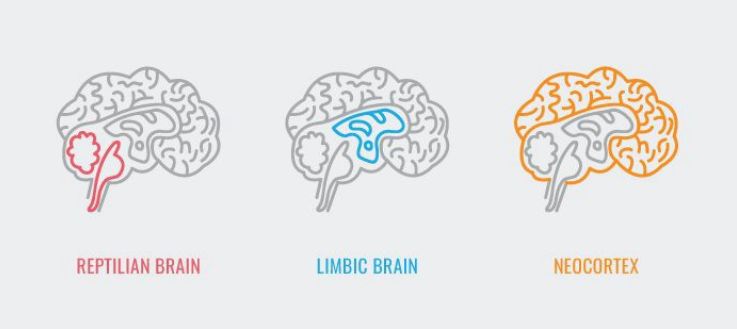
The brain stem (the reptilian brain) and the limbic system together make up what we call the emotional brain, the oldest part of our brain.
The emotional brain is responsible for emotions, regulating arousal, attachment and connection to others, survival and wellbeing, and is what gives the fight-flight-freeze response when we think we are under a threat.
The neocortex (including the prefrontal cortex) is the highest and youngest part of the brain, and is what we call the rational brain. It is responsible for “think and reason”, taking in information from the outer world, language, imagining, learning, making choices, empathy and mindfulness. The prefrontal cortex specifically is responsible of the integration of the whole body-brain-outer world system. It lets us go from chaos, rigidity or withdrawal, to harmony, understanding and calm within ourselves and also outside with others. So this part of the brain basically down regulates the emotional brain.
Normally the emotional and rational brains work together. They are connected. The emotional brain takes in and sends information faster than the rational brain (ex: you think you saw a snake). You might react at first, jumping away, and when you see it wasn’t a snake, your rational brain down regulates and you relax. (Another example: You thought a friend was unkind, then you realized she was having a bad day and it didn’t have anything to do with you.)
At other times, we might get triggered, and we might flip the lid, losing the connection between the prefrontal cortex and the emotional brain. This is when we are ruled by our emotions, we might say things or act in ways we normally wouldn’t, losing contact with reasoning, perspective, humor, compassion, empathy or moral behavior. We are disintegrated. We might feel really stuck, small and disconnected. (Example: You were having a bad day, you thought a friend was unkind and you overreacted.)
What we need in those moments is to (1) recognize that we have flipped the lid, and just this recognition alone can start the reintegration process, and (2) connect the prefrontal cortex to the emotional brain again with mindfulness of all present thoughts, emotions, sensations, and the outside world. Connecting them together, attending to what’s going on, kindly befriending all aspects of it, integrating ourselves.
Trauma and mindfulness
Traumatic stress is different from the usual meaning of the word stress.
An estimated 90% of the population has been exposed to a traumatic event, after which people can develop post traumatic stress. If the stress persists for longer than a month, it might be diagnosed as posttraumatic stress disorder (PTSD), which impacts 8-20% of the population exposed to any traumatic event.
Trauma can be any event that leaves us feeling helpless, unsafe or overwhelmed. Examples are natural disasters, accidents, violence or abuse. Trauma can also occur by second-hand exposure (if you witness trauma) and by continuous microaggressions (being targeted by systems of oppression, for example, if you are poor, working class, disabled, a person of color, transgender, a woman).
Traumatic stress can be triggered even if some time has passed since the event.
Trauma happens due to a disconnect between the emotional brain (which gives the fight-flight-freeze response) and the rational brain (which processes the memory of the event and understands what’s happening). The emotional brain keeps signaling to the body that it is still under threat, even if the event has passed and the person is no longer under threat. The body cannot restore a sense of stability and safety. The content of the traumatic event is less important than the fact that the event could not be integrated, and the person is still suffering.
It is possible to integrate the traumatic experience and heal from traumatic stress.
Mindfulness practice has been scientifically proven to help heal from trauma by
- enhancing present moment awareness,
- enhancing body awareness,
- enhancing the ability to self-regulate,
- and increasing self-compassion.
Research also shows that mindfulness practice can at times exacerbate trauma symptoms by inviting trauma survivors to come into contact with the traumatic stimuli. In other words, mindfulness practiced without an understanding of trauma can increase stress rather than decrease it. This is why we emphasize an understanding of trauma in this course and all other mindfulness practices.
Recognizing signs and symptoms of trauma
Trauma lives in the body and is complex. It can show itself differently in different people. Symptoms of traumatic stress can include:
- flashbacks / a repetition of the sensory stimuli related to the traumatic event (thoughts, sounds, images, sensations, emotions)
- nightmares or difficulty sleeping
- avoiding any reminders of the trauma (avoiding the place it happened, avoiding related people etc.)
- heightened emotional arousal (such as fear, anxiety or irritability)
- intrusive thoughts or images
- dissociation (disconnect between one’s thoughts, emotions and physical sensations, a sense of leaving the body or being far away)
- loss of appetite
- social isolation
- difficulty concentrating.
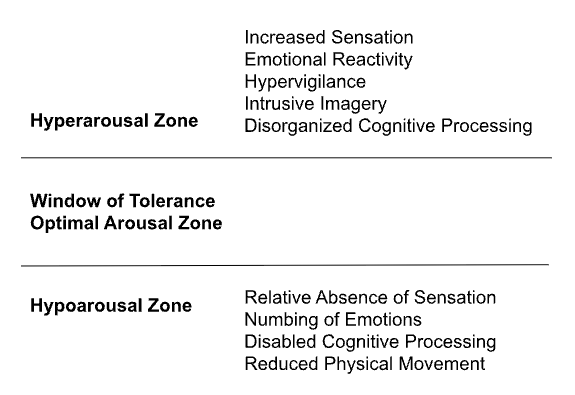
Trauma survivors might experience swings between hyperarousal (continuous flood of sensory stimuli and sensations) or hypoarousal (getting cut off from our senses), as shown in the image below:
Practicing mindfulness in a trauma-informed way
We practice mindfulness to relieve suffering, not to intensify it. In other words, we want to try to stay within our window of tolerance when practicing mindfulness. This is where we can integrate the traumatic stress, tolerate our emotions and find healing.
Another way of saying we want to stay in the window of tolerance, is saying we want to stay in the River of Integration. See image below:
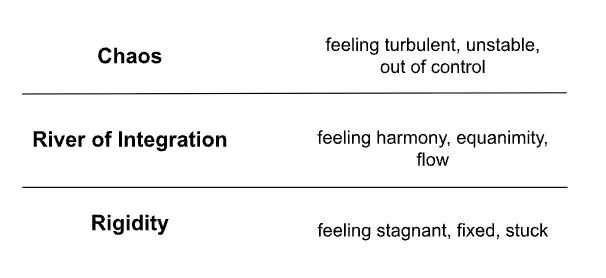
Yet another way of saying we want to stay in the window of tolerance, is saying that we want to stay in the Discomfort Zone. This is where learning happens. If we are in the Comfort Zone, we might not be learning, and if we are in the Alarm Zone, we won’t be learning either because we will be overwhelmed by our experience. We want to keep ourselves in the Discomfort Zone.
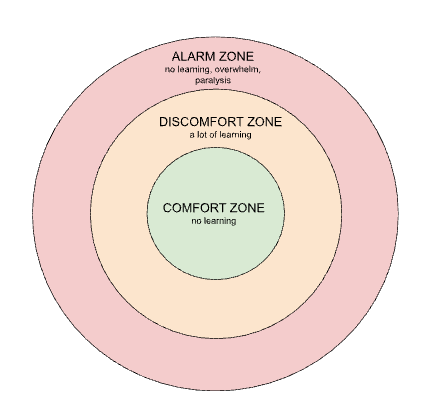
Any moment we sense that the practice is increasing our suffering, we are losing a sense of safety and stability, we are moving above the window of tolerance (hyperarousal) or below it (hypoarousal), we need to respond appropriately and pause the practice.
Research shows that trauma survivors have a tendency to focus on trauma-relevant stimuli. Plus, due to an emphasis on the many positive effects of mindfulness and upon encouragement from teachers who are not trauma-informed, trauma survivors might insist on practicing mindfulness even when they are stressed, which might create a threat of getting retraumatized.
It is important to remember that easy does it. You can pause the practice as many times as you need and build your meditation practice very slowly over the next months and years with a kind and steady effort. (See modifications below)
The good news is that your window of tolerance is not static and it will naturally and gradually expand over time. With a slow and gentle practice, you will notice that you’ve become able to tolerate more and more of the difficulties that come up in your life. This will be the joyful fruit of staying with meditation in a soft and steady way.
Practitioners who experience these adverse effects during practice often feel ashamed, isolated and scared to talk about what they are experiencing (especially when everyone else seems to be sharing how relaxed, calm and wonderful they feel after meditating!). If you have any questions at any moment, please feel free to reach out to me.
Trauma sensitive modifications to your practice
It is possible to learn and practice mindfulness while being safe and stable by putting in place the following modifications:
Discovering your own window of tolerance
You might find it helpful to discover how traumatic stress lives in your body and recognize which symptoms signal to you that you are outside your window of tolerance. A steady mindfulness practice will help you become more aware of your body and the sensations in your body. You will, over time, become more aware of your window of tolerance.
You might also avoid any obvious areas of overwhelm in your life: a very difficult relationship in which you suffer a lot, an area where you sense there is a strong tangle. You can start resting your attention on things that are uncomfortable or difficult, while also being manageable and workable.
An attitude of courage can help. Discovering what hurts too much might mean you come into contact with some pain. It might feel like you’re walking across a dark room full of furniture, and even though you are walking super slowly, you still sometimes hit a knee or elbow. This slight pain is a natural part of discovering your boundaries. You might courageously welcome this pain, and be quick to offer this hurting part of you the protection it needs.
An attitude of patience can help as well. You might remind yourself that your window will naturally expand over time; there’s no need to go faster.
When you notice a difficulty coming up, you can assign it a value of difficulty on a scale from 1 to 10. You can imagine that 10 is the extreme end of being above your window, and 1 is the extreme end of being below your window. You can track to see if you are staying in the middle part, on difficulties that seem like a 4, 5 or 6.
Staying within your window of tolerance
When you develop an awareness of your window of tolerance, any moment you notice you are above or below it, you might find it helpful to pause the practice by
- opening your eyes,
- naming objects you see in the room (“I see blue flowers, I see a chair...”),
- leaving the room,
- going out for a walk,
- distracting your mind from what triggered you by going over your grocery list or watching a short video,
- searching for areas in your body that feel safe and stable,
- finding external resources (hugging someone or your pet, connecting with a friend etc.),
- going back to your inner resources (places or beings that bring you a sense of safety and comfort, a compassionate touch on your heart or belly, compassionate phrases, a few slow deep breaths, grounding yourself to the Earth etc.).
Going slow
You might find it helpful to engage in shorter practice periods and build your mindfulness practice very slowly over time (for example: 5 minutes a day over 3-4 months, increasing to 10 minutes only when you sense that you can).
Practicing resilience and self-compassion first
You might find it helpful to practice only self-compassion meditations for a long time (lovingkindness for the self, resourcing), before you feel safe and stable enough to open up to a larger mindful presence. You can choose to start your daily meditations by practicing self-compassion first (for example, doing 5 min of Resourcing before an Anchoring practice).
Practicing in relationship rather than practicing alone
We can’t heal trauma in solitude; research shows that social support is critical in healing. You might want to practice mindfulness with a teacher, a community or a person you trust and feel safe with, or with a trauma professional who also is trained in mindfulness.
Finding an anchor that works for you
If anchoring on the breath is not possible or too difficult, you might want to anchor okn sounds, on hands, on feet, on touching a soft blanket or on the sensations of walking. I will support you to find the best anchor that works for you.
Practicing with movement
If you don’t feel a lot of sensations in the body (you feel numb or checked out), you might find it helpful to incorporate movement (walking, yoga, stretching) before or during your practice. You might also find it helpful to practice mindfulness in standing or walking postures, rather than sitting.
Seeing a trauma specialist
If you are seeing a therapist, you might want to inform them about your enrolment into a mindfulness program so that they can support you accordingly. You might want to ask if your therapist has a specialty and training in trauma. If you are not seeing a professional, you might find it helpful to consult a trauma specialist, as expertise and the presence of a safe relationship is critical in healing from trauma. (see some references below)
Exploring 1:1 practice with a teacher
You might find it helpful to practice 1:1 with a mindfulness teacher to ensure you stay within your window of tolerance and build up your presence slowly over time. (Happy to assist you with this or refer you)
References
- “Trauma Sensitive Mindfulness” by David Treleaven. 2018.
- “Body Keeps The Score” by Bessel van der Kolk. 2015.

